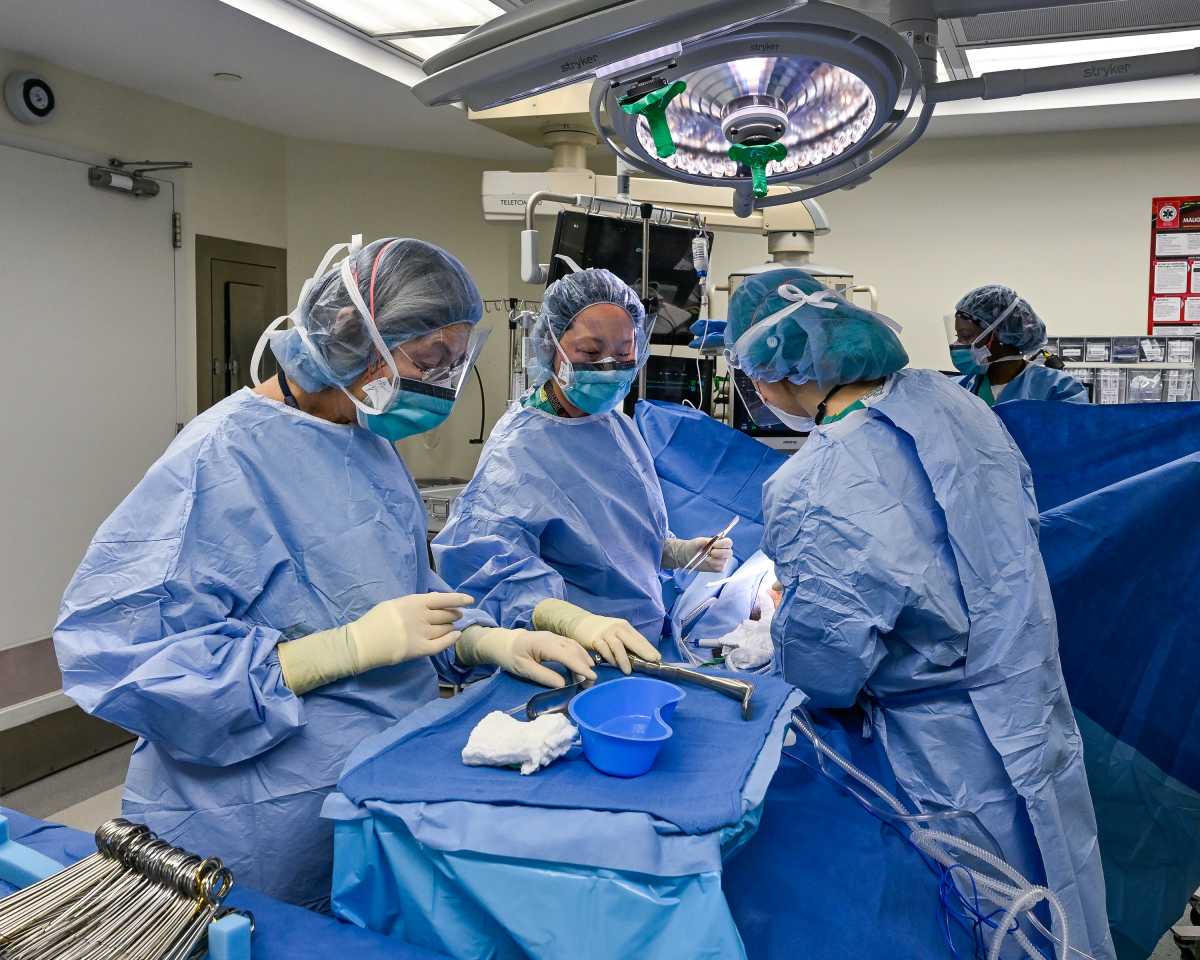
March may be known for celebrating Women’s History Month, but it’s also a critical time to spotlight a rising health threat: colorectal cancer. Some of the female doctors leading the charge say that screening is more important than ever, even for younger adults.
In an interview with Maimonides Health physicians, Dr. Julie Yang, director of the Comprehensive Cancer Gastroenterology program, and Dr. Rebecca Rhee, division chief of Colorectal Surgery and program director for the General Surgery Residency, highlighted the importance of female representation in a still male-dominated field. According to the American Journal of Gastroenterology, only 18% of practicing gastroenterologists are women, and just 3% of gastroenterology fellows are female.
More importantly, both stressed the need for colorectal cancer screening, even in younger adults.
The American Cancer Society (ACS) estimates that in 2026 alone, approximately 108,860 patients will be diagnosed with colon and rectal cancer, with about 55,230 deaths.
Most alarming, the doctors noted, is that colorectal cancer is on the rise in people under 50 by nearly 3% per year and is now the leading cause of cancer-related death in this age group.
Dr. Rhee, who graduated from medical school in 2007 and has been at Maimonides for 13 years, told Brooklyn Paper that while hereditary colon cancer increases the risk of colorectal cancer, the majority of patients under 50 diagnosed with the illness do not have any hereditary or genetic link. While nobody knows for certain the cause of the rise, sedentary lifestyles, overweight and obesity, smoking, heavy alcohol use, low-fiber, high-fat diets or diets high in processed meats, and other environmental factors have all been associated with the disease.
“If you were born in the 1990s, you are at increased risk for colorectal cancer, even 50% more likely than people who were born before that time,” Dr. Rhee said, noting that colorectal cancer among adults under 50 is increasing worldwide.
However, there is still stigma and misconceptions surrounding colon cancer screening. Patients are either too embarrassed to address symptoms with their doctors, feel that the procedure is “too intimate or invasive,” or are deterred by the bowel preparation, which involves drinking a large amount of laxative solution and frequent trips to the bathroom.
Test options for colorectal cancer screening range from noninvasive stool-based tests, such as Cologuard, to CT colonography and colonoscopy. With advances in technology and medicine, preparation and procedure for colonoscopies have become less invasive, minimizing patient stress and anxiety.
“I’ve done it myself,” Dr. Rhee shared. “The procedure is absolutely nothing. It’s so brief, you’re comfortable, you feel great when you wake up. The prep is, of course, a little intense, but it’s totally fine. So it’s just really trying to get over that fear. There are also stool tests that can be performed, such as Cologuard. They are very reliable, [and] if the Cologuard test is positive, you definitely need to get a colonoscopy.”

Dr. Yang, a practicing gastroenterologist for 15 years whose specialty is gastrointestinal cancers, told Brooklyn Paper that the “hottest topic” in gastrointestinal medicine is the early onset of colon cancer.
“There is a rise in the past decade of the 50-and-under age group having colon cancer and dying from it. We’ve decreased mortality from colon cancer, particularly in the older age [group]. But for some reason, we’ve seen a rise in early-onset cases in the past decade or so. We don’t understand why,” Dr. Yang said.
Recently, the ACS lowered the age for regular colon cancer screening from 50 to 45. If colorectal cancer is caught early, the five-year survival rate is 90%. During a colonoscopy, doctors screen for abnormalities in the colon’s tissue and identify cancerous lesions or polyps, which they remove and send in for testing. All colon cancer comes from polyps, which can take as long as 10 to 15 years to develop into cancer or be detected in its early stages.

Dr. Yang stressed the importance of early screening because colon cancer is more than 90% preventable. She explained that during a colonoscopy, doctors not only check for abnormalities in the colon’s tissue and cancerous lesions but also for pre-cancerous polyps, the major cause of colon cancers.
“Whether you have symptoms or not, you should go to your doctor and just inquire about your screening colonoscopy and check for colon cancer,” Dr. Yang explained, noting that, regardless of age, people should watch for symptoms like rectal bleeding; changes in bowel habits, such as diarrhea, constipation, or narrowing of the stool; abdominal discomfort, including ongoing cramps, gas, pain, or a feeling of bloating/fullness; and symptoms of anemia, like unexplained fatigue, easy tiredness, and lethargy.
“For us as gastroenterologists, our biggest fight, whether it was early onset or not, is to just get people comfortable with the idea that you have to screen for colon cancer. We feel so passionate about it because it is a preventable cancer, versus other cancers where there’s no pre-cancerous or pre-set lesion that we can follow that’s predictable,” she said. “We’re just here to dispel the rumors that it’s not as horrifying as people think; it’s not like a horror show movie. It’s very easily done, and there are lots of different options to get colon cancer screening if you can’t get a colonoscopy, which is just as appropriate.”
39-year-old mother of two Tammy Smith shared her colon cancer journey with Brooklyn Paper.

The former Alabama resident had a long history of symptoms like IBS, bloating, prolonged constipation, and rectal bleeding. Doctors in Alabama dismissed her symptoms, telling her the bleeding was due to hemorrhoids and prescribing hemorrhoid medication and laxatives.
Her sister, a nurse, urged her to get a colonoscopy, suspecting Crohn’s disease. Smith eventually had a CAT scan and an MRI in Alabama, which doctors misdiagnosed.
“I don’t know how they even missed it,” Smith said.
It wasn’t until Smith visited her family in New York City four years ago that she was diagnosed with stage 4 colon cancer.
She recalled that after being unable to eat for a week, she went to Maimonides, where doctors immediately ordered testing and found not only colon cancer but also spots on her liver and lungs.
“I was in Alabama when this was happening, and I just don’t think the right doctors were looking at me, because as soon as I went to Maimonides that same night, I found out something was wrong,” Smith shared, praising the doctors at Maimonides for their professionalism and patient care.
Dr. Rhee was Smith’s colorectal surgeon. Rhee focuses on minimally invasive surgical techniques to help patients recover more quickly and achieve the best possible outcomes. Smith recalled Dr. Rhee’s confidence when she met her, who reassured Smith that she was “going to be just fine.”
“[Dr. Rhee] really fought for me. She wanted to save me. She told me that when she first walked in while I was in the hospital, ‘I’m gonna work on you, I’m gonna save you,’” Smith shared, describing the doctor as a beautiful soul. “I was like, ‘Oh my God, this is a confident lady.’ She took a little bit of anxiety from me. I mean, I was scared to death, but I had never seen a doctor walking that confidently like that ever before.”

Smith, a former postal worker who had planned to become a postmaster before her diagnosis and had to quit her government job due to her illness, is in remission.
After her diagnosis, Smith extensively researched colon cancer and found that the subject is still taboo, particularly in Black and Brown communities. She stressed the importance of early education about colorectal cancer and screening.
“I didn’t see any Black young females talking about [colon cancer],” Smith shared. “When I looked it up, I saw a lot of 50-year-old white men, you with rectal cancer [and] colon cancer. I didn’t know anything about it. We have to educate ourselves and get familiar with this, because it’s happening more to younger people.”
Smith, who is celebrating her 40th birthday next month and planning a trip to Orlando with friends, suspects her cancer was due to environmental influences since a cancer DNA test was negative for cancer risk genes. While living in Alabama, she resided in an area where residents were exposed to pollutants from oil refineries and shared that many of her neighbors were diagnosed with various forms of cancer.
“I don’t know if it was just in my area, because there’s a lot of oil plants out there in Alabama, but a lot of people started getting cancer in the area as well. That makes it even more serious. That means it was environmental. That’s why a lot of people are getting it,” Smith noted. “More people need to know. I think younger Black people, especially in my community, like in Alabama, no one gets checked. The doctors ain’t even checking them properly there. There were so many people who died of cancer in the same community, around the same time I got cancer; it was so many people dying of cancer.”