Breast cancer is the second leading cause of cancer deaths in women, and a diagnosis can be scary and isolating. But, for decades, organizations like Maimonides Medical Center, the National Breast Cancer Foundation, NYU Langone Hospital – Brooklyn, and the Susan G. Komen Foundation have partnered with local communities to support breast cancer survivors and those living with the illness in support of National Breast Cancer Awareness Month in October.
Breast cancer is a form of cancer in which abnormal cells grow rapidly in the breast tissue and can spread to other parts of the body if the individual does not seek treatment. Each year about 240,000 new cases of breast cancer will be diagnosed in women and 2,100 in men. Roughly 42,000 women and 500 die of breast cancer each year. Out of all cases, Black women are the most likely to die of the disease.
Like all cancers , breast cancer is caused by a genetic mutation in cells. Some individuals may be at a higher risk of developing breast cancer because they have inherited cancer-causing genes like the BRCA1 or BRCA2 gene, but other factors contribute to the likelihood of developing the disease — like age, family history, reproductive history, genetic mutations or previous history of breast or ovarian cancer.
While those risk factors are things an individual cannot change, there are some things that one can change about their lifestyle to reduce the risk.
“We know that women who are heavier or obesity, for example, increases breast cancer risk,” Dr. Nina D’Abreo, division chief of hematology and oncology at NYU Langone Hospital—Brooklyn told Brooklyn Paper. “Certain lifestyle changes, for example, drinking alcohol — even one drink a day increases the risk of women’s breast cancer in her lifetime. Those are things we can change.”
Some other modifiable factors include regular exercise and the avoiding use of long term postmenopausal hormone replacement therapy if possible.
One extremely important factor in maintaining overall health and mitigating breast cancer risk is by regularly visiting a physician and regularly scheduling mammograms after the age of 40.
“We know that despite all of those modifications, the best way to detect breast cancer is through screening,” D’Abreo said. “For women who are what we call ‘average risk’, [who] don’t have any of these higher risk factors and family risk factors, mammographic screening should start at age 40 and we usually recommend [screening] once a year.”
A mammogram is essentially an X-ray for the breast. Doctors use mammogram scans to detect any abnormalities within the breast tissue and early signs of breast cancer. With mammograms, physicians can detect breast cancer much earlier than just through the patient feeling for any physical changes in their breasts.
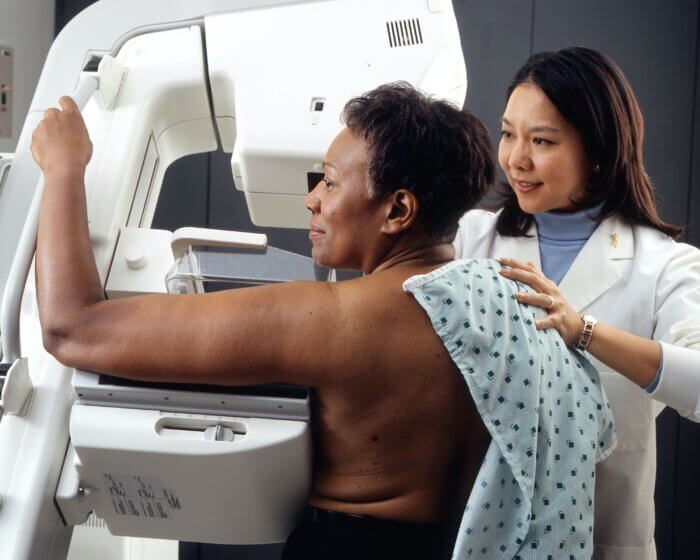
The images are are taken by placing each breast on the plastic plate of the mammogram machine. The breast is then compressed by the machine and several images are taken and then observed by a physician for any abnormalities in either breast.
Some patients report pain or discomfort during the procedure, but overall it is not harmful and there are several steps you can take to minimize any discomfort with a physician.
Although the procedure can be uncomfortable or painful, it is extremely effective at detecting any potential cancer in the breast and can detect breast cancer up to three years before the individual would themselves notice any changes to their breast.
One of the largest obstacles to diagnosing and treating breast cancer is not scheduling regular mammograms. Waiting too long to get screened or avoiding it completely can be dangerous as over time, potential cancers can grow or metastasize — meaning they spread to other parts of the body.
“I do admit that this is the hardest thing to get everybody [screened],” said D’Abreo. “But it’s trying to figure out what the fear is and then trying to find out what exactly is preventing somebody from getting that screening. Sometimes it’s the fear of not wanting to know that they have cancer. That we’ve seen happen time and again, so speak to your doctor. We can come up with strategies.”
If an abnormality does show up on a screening, the next step is to biopsy the abnormality or mass to see if the cells are cancerous. If they are, the patient will then meet with a breast surgeon to see what surgical steps should be taken to remove the cancer. Following potential surgery, the patient will meet with an oncologist to design a treatment plan to shrink any remaining cancerous cells.
“The way to think about this is you’re not just taking the seed out of the breast, you’re also treating the body because having breast cancer on its own in the breast is not the problem,” D’Abreo said. “It’s really the concern that this breast cancer, if not appropriately treated, can come back and spread to other parts of the body.”
Even after a patient has undergone a mastectomy, or a surgery removing the breast tissue, there’s still about a 1% chance of having breast cancer or having the cancer return. The risk isn’t zero even after surgery because it is incredibly difficult for surgeons to completely remove every single cell of the cancer or the breast tissue.
This is why both men and non-binary individuals are also at risk for developing breast cancer. If a non-binary individual who has already undergone top surgery to remove breast tissue has either BRCA genes or has a family history of breast cancer, they are still at risk of developing the disease.

For men or non-binary individuals, screening for breast cancer looks a little different. Instead of a mammogram, physicians rely on the use of regular physical examinations and an ultrasound or MRI scan to look at the area.
“So the mammogram is an X-ray of the chest, so if you’ve had a mastectomy [or top surgery] we are examining what we call the chest wall,” said D’Abreo. “It is actually easier to feel things if they are on the chest wall, the breast is essentially a big lump of fat, if you will, and once you take that off and you haven’t had reconstruction, you can see your chest wall.”
Regardless of gender, if an individual is at higher risk of developing breast cancer, it is extremely important to form a good relationship with their physician and – if applicable – schedule regular screenings and checkups to make sure that their health is being monitored.
“I think the main thing is to make sure that people get screenings and not to be afraid of screenings, but to ask questions,” D’Abreo said. “There are a lot of myths out there, there’s information and misinformation. So don’t be afraid to ask questions.”























