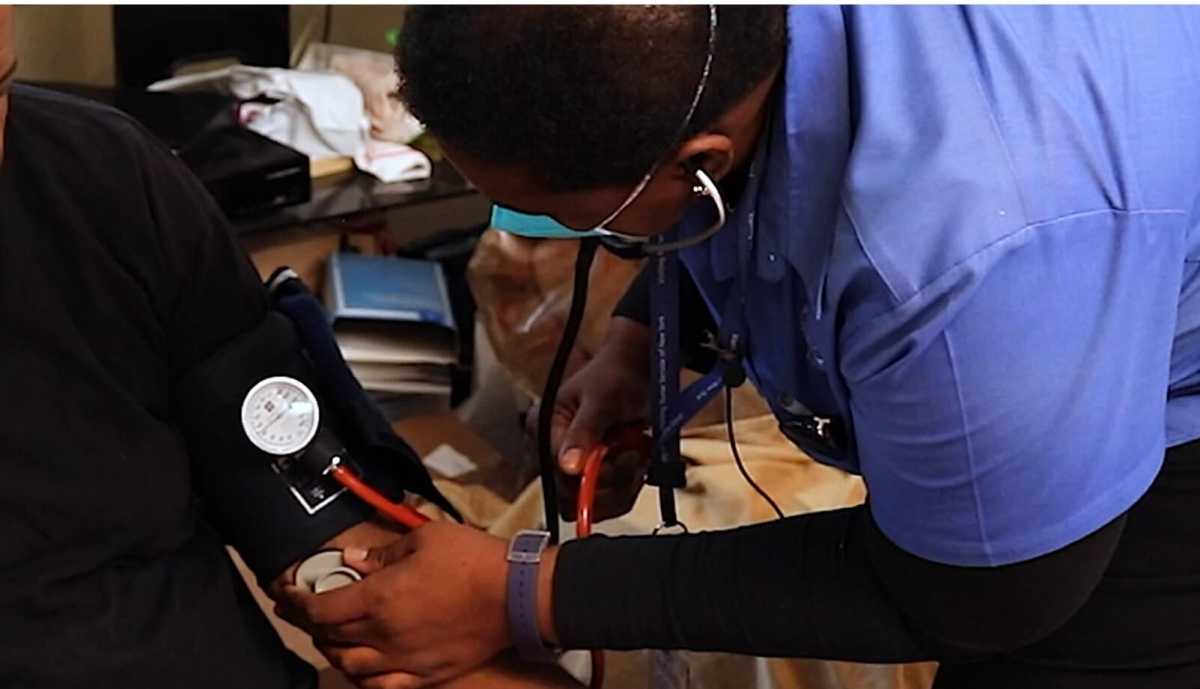
Sherill Stennett, a home care nurse with Visiting Nurse Service of New York, spends her days making rounds that look a little different than the ones most often associated with nursing. Rather than walking down a hospital hallway to check in on her patients, Stennett travels through Brooklyn to care for her clients in their own homes.
Stennett has been a home care nurse for two decades, and has spent all but one of those years working with VNSNY. She got started as a nurses’ aide in a hospital, where her colleagues, impressed by her skills, encouraged her to go back to school.
She did, enrolling in a program to become a Registered Nurse and then, while she was at it, earned her Bachelor of Science in Nursing. But, rather than heading back to the hospital for a career there, Stennett took inspiration from the time she had spent caring for an elderly family friend in their home and turned toward home care.
“Most of these patients are homebound and have challenges leaving the home, it’s very difficult for them to go outside of the home to get care,” she said.
Stennett and her colleagues will usually care for a patient for about four to five weeks, and she loves being able to see a patient through their entire course of treatment, until her services are no longer needed.
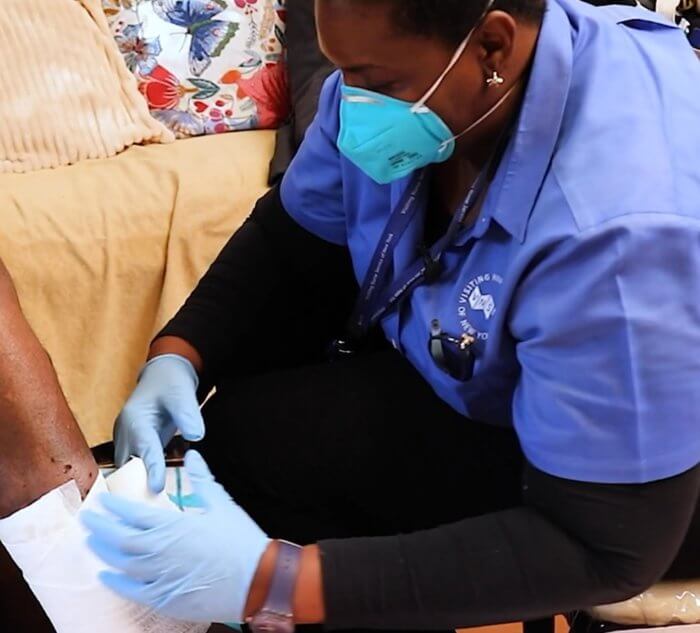
“In the hospital, they’re there for a couple of days, and you wonder ‘Oh, I wonder how Mr. X. is doing … how are they coping? When you’re in the home, you get the whole entire picture,” she said.
The continuity of care matters, she said, and so does taking in every element of a patient’s life. At the hospital, the doctors and nurses can write down all of their recommendations and advice, but it’s out of their hands as soon as the patient walks out the door.
“You can do a cupboard run, oh let’s see what’s in your cupboard, does it match [the recommended diet,]” Stennett said. “Let’s see your grocery list, you pop in the day they deliver the groceries and you can say ‘Oh no, this isn’t good for your diet.”
Patients instructed to eat less sodium, or fewer carbs might not know how to translate that advice into their everyday lives, and that’s where the home care nurse homes in — teaching them how to read labels, what to avoid and what to embrace.
“It’s not like we’re going in and just taking over … there’s a lot of teaching,” Stennett said. “Yes, we deliver quality care, but our aim is always to leave them as independent as possible. It’s more hands-on, more realistic, and the end product is a better outcome.”
Home care has also been a better outcome for Stennett — early in her career, when she was working in the hospital, she left for the hospital at 6 am and usually didn’t return until after 8 pm, giving her nearly no time with her children. Once she made the shift, she had shorter, more flexible working hours and more time for herself.
It may seem isolating, but working out in the field isn’t really so different from having a team of nurses surrounding her in the hospital, she said. If one nurse is in a patient’s home and realizes they’ve run out of something they need, they can send a message out to colleagues and know that someone else can come drop it off — the same is true if they’re having trouble managing a patient by themselves. Someone else is always around to help.
Home care during the pandemic
Being outside of the hospital didn’t cushion the impact of the pandemic, Stennett said.
“We were very fearful,” she said. “Nobody knew what was going on, nobody knew what to expect.”
VNSNY quickly outfitted their nurses with Personal Protective Equipment and set up a support number for staff. A mask policy for patients was put in place — care could not be given unless they were masked.
“You felt isolated because you’d be outside and there was nothing going on outside, you were fearful of going in and out because you don’t know what you’re going into,” Stennett said. “We got that support, that made a big distance. But it was scary — it was terrifying, in the beginning. Now, we have adjusted to the new norm.”

Nursing is challenging, but it’s nothing she can’t handle — especially with support from her colleagues and managers. If she was given the opportunity to return to nursing in the hospital, she’d turn it down, she said.
“I’ve had challenges but I was given the support to deal with it,” she said. “I haven’t had anything that has deterred me from working.”
Of course, Stennett and her colleagues are being celebrated this month for National Nurses Week and National Nurses Month.
“It’s great to be part of a great nursing body as VNS,” she said. “I must say, we all work together, the nurses. We look out for each other.”
This week, they gathered for a meeting to recognize their hard work, and next week VNSNY will host two separate celebrations to ensure all of their nurses can get in on the action, Stennett said.
“We are celebrated, and it’s good to be celebrated and recognized for the work we do.”